Since our inception in September of 1996, IEHP has successfully met the health care needs of the community. Today and into the future we remain committed to continually exploring innovative ways to meet changing healthcare needs.
Since our inception in September of 1996, IEHP has successfully met the health care needs of the community. Today and into the future we remain committed to continually exploring innovative ways to meet changing healthcare needs.
2023 Covered California enrollment opens. IEHP Covered is I.E.’s Lowest Cost Silver Plan.
2021 IEHP Foundation is established. Their mission is to inspire and ignite the health of the Inland Empire.
2019: IEHP Chief Operating Officer Jarrod B. McNaughton was appointed as Chief Executive Officer effective July 20.
2019: IEHP Chief Executive Officer Dr. Bradley P. Gilbert retires after a distinguished career on July 19.
2019: IEHP celebrates the groundbreaking ceremony for the new Dr. Bradley P. Gilbert Center for Learning and Innovation.
2018: IEHP evolves its five strategic priorities into two new areas of strategic focus: The Health of the System and The Health of our Members, as part of its continuing drive to become a 5-star health plan.
2017 Helping Hearts is launched. Volunteers from IEHP donate thousands of hours to this program and various charities over the years.
2017: IEHP is lauded as the first health plan in the nation to reach 25,000 Medicare-Medicaid members.
2017: IEHP creates the fourth Super Hero, Mighty Fitnessa, to include fitness in our promotion of healthy, active lifestyles.
2017: IEHP opens the second Community Resource Center in Riverside.
2016: IEHP launches five strategic priorities to drive IEHP toward its goal of becoming a 5-star health plan.
2015: IEHP implements LEAN principles of leadership, to guide quality improvements and positive change.
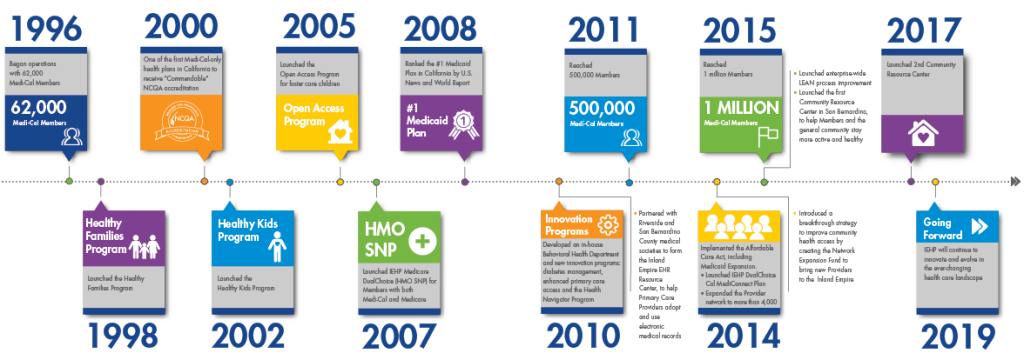
2015: IEHP reaches the 1 Million Member Milestone.
2015: IEHP launches the first Community Resource Center in San Bernardino to help Members and the general community stay more active and healthy.
2014: Healthcare reform policies are implemented across the nation and the Cal MediConnect Plan. In the Inland Empire, more than 350,000 Inland Empire residents will become eligible for health coverage through the Medi-Cal expansion, over 530,000 residents will be eligible for the Health Exchange, and 80,000 residents will be eligible for the Cal MediConnect Plan.
2011: Seniors and people with disabilities who have Medi-Cal are required to enroll into managed care.
2010 IEHP becomes the first health plan in the state to bring behavioral health coordination in-house.
2010: IEHP launches new Innovation Projects — Diabetes Management, Enhanced Primary Care Access, and the Health Navigator Program. In June, the Health Navigators began home visits to help members better navigate the health care system.
2009: IEHP creates the third Super Hero, Super Nutricia, to rescue kids from the evils of junk food and promote healthy-eating habits.
2008: IEHP is ranked the #1 Medicaid Plan in California by U.S. News and World Report.
2007: IEHP launches a Medicare Special Needs Plan, IEHP Medicare DualChoice (HMO SNP), for people with both Medi-Cal and Medicare.
2006: IEHP is recognized by the Managed Risk Medical Insurance Board (MRMIB) as a top-enrollment entity for the Healthy Families Program.
2005: IEHP launches the Open Access Program for foster care children in San Bernardino County.
2003: IEHP partners with Riverside and San Bernardino counties to develop the award-winning program, Open Access, for foster care children.
2002: IEHP forms the Persons with Disabilities Workgroup (PDW) for members with a disability to share their experiences and help IEHP improve its services.
2002: IEHP launches the Healthy Kids Program, for low-income uninsured children who do not qualify for Medi-Cal or Healthy Families.
2001: IEHP creates the second Super Hero, Eradicator, to lead a community-wide, anti-smoking campaign for children.
2001: IEHP is ranked the 9th largest Medicaid Plan in the United States.
2000: IEHP becomes one of the first Medi-Cal only health plans in California to receive "Commendable" NCQA Accreditation.
1998: IEHP launches the Healthy Families Program, for uninsured children in working families who do not qualify for Medi-Cal.
1997: IEHP creates the first Super Hero, Rad Rider, helping children learn important bicycle safety rules.
1997: IEHP establishes the Public Policy Participation Committee (PPPC) for members to give feedback and voice their opinions.
1996: IEHP begins operations with over 60,000 Medi-Cal members.
1994: IEHP is established as the local initiative, not-for-profit Medi-Cal Managed Care health plan in the Inland Empire.
1993: California shifts the delivery of Medi-Cal from mainly fee-for-service to a managed care system.